Did you ever get chickenpox as a child? If so, you’re at risk of developing shingles later in life. How do you recognize shingles, and what can you do to avoid complications? Read on for the answers to these questions!
What is shingles?
Like chickenpox, shingles is caused by the varicella-zoster virus. As a result, many people believe that shingles is similar to chickenpox. But that’s not exactly true. The two diseases do not present in the same way or at the same time in life. For instance, chickenpox is typically a childhood illness, whereas shingles mostly affects adults and seniors.
Does your child have chickenpox?
Don’t panic! Read our tips for treating chickenpox
What causes shingles?
After a person recovers from chickenpox, the virus remains dormant (asymptomatic) in their body for many years. Later in life, the virus can reactivate and cause shingles.
About one in three people will develop shingles at some point in their life. It’s important to note that you can’t get shingles unless you’ve already been infected with the chickenpox virus in the past.
Who is at higher risk of developing shingles?
Although anyone who has ever had chickenpox can develop shingles, some populations are at greater risk:
- Adults aged 50 and over
- Immunocompromised people (people with a weakened immune system)
- People with certain chronic diseases, such as rheumatoid arthritis, lupus, inflammatory bowel disease, chronic lung or kidney disease, and insulin-treated diabetes
What are the early symptoms of shingles?
When the shingles virus reactivates, it affects a specific area of the skin and usually appears on just one side of the body. The first symptoms of shingles are usually a burning or tingling sensation in the affected area, before the rash appears.
What does shingles look like?
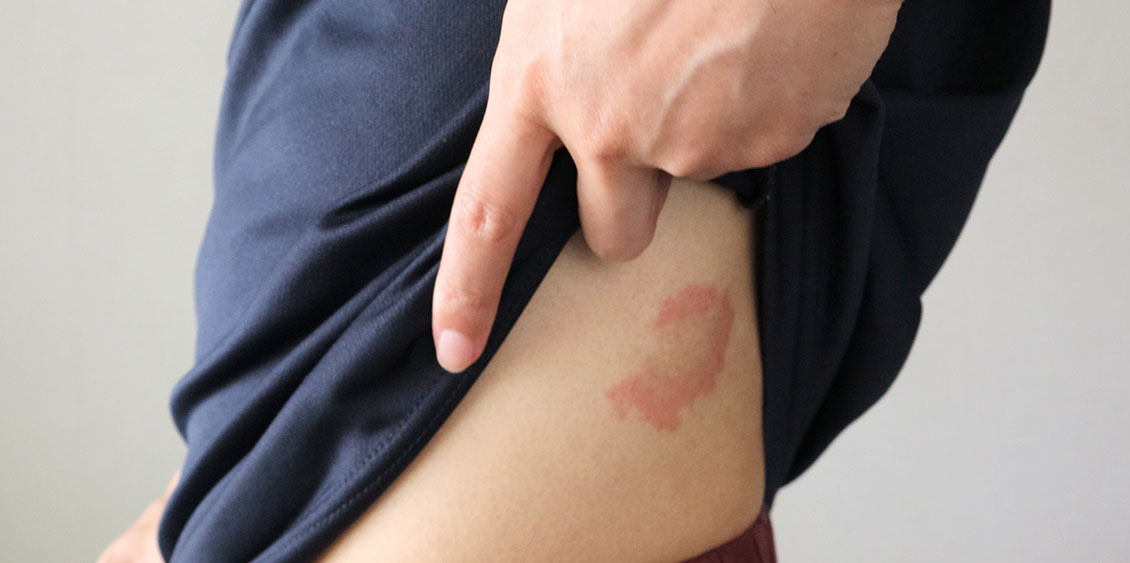
One to three days after the first symptoms, red patches and small fluid-filled blisters appear in clusters, often causing intense pain and itching. The blisters dry out and go away on their own within two to three weeks.
What are the possible complications of shingles?
Unfortunately, pain and burning may persist after the blisters have healed. This is known as post-shingles neuralgia, and it’s the most common complication of the disease. This pain often feels like electric shocks in the area affected by shingles. It can last from a few weeks to several months and, in rarer cases, can even persist for life.
This pain can seriously impact quality of life, causing:
- Fatigue
- Insomnia
- Depression and anxiety
- Loss of appetite
- Social isolation
More rarely, post-shingles neuralgia can also lead to hearing or vision loss, facial paralysis, or skin superinfection.
Prompt treatment helps to reduce the risk of complications. It’s important to recognize the symptoms and consult your doctor or pharmacist promptly if you think you have shingles.
Is shingles contagious?
The fluid in shingles blisters can transmit chickenpox to someone who has never had it, but it cannot transmit shingles directly. In addition, the blisters are no longer contagious once they have crusted over.
If you’ve never had chickenpox and you touch the fluid-filled blisters of someone with shingles, you could catch the virus and develop chickenpox. That’s why handwashing is essential to help prevent transmission. It’s also best for certain populations to avoid contact with anyone who has shingles—especially pregnant women, as there are risks for both mother and baby.
Vaccination: The best means of prevention
The shingles vaccine remains the best protection for several reasons:
- It reduces the risk of developing shingles and of developing related complications.
- It reduces the intensity of symptoms if you do develop the disease.
- It reduces the risk of recurrence for people who have already had an episode of shingles in the past.
This vaccine is administered in two doses. Once you’ve received both doses, the vaccine maintains its efficacy, so there is no need for a booster.
Who is eligible to receive the shingles vaccine?
The shingles vaccine is recommended for anyone aged 50 and over. It is also recommended for those with a weakened immune system due to a disease or treatment, as well as people living with certain chronic conditions (rheumatoid arthritis, lupus, chronic inflammatory bowel disease, chronic lung or kidney disease, or insulin-treated diabetes).
In Quebec, the shingles vaccine is offered free of charge to people aged 71 and over, as well as to immunocompromised adults. Elsewhere in Canada, eligibility criteria may vary from province to province. For those who do not qualify for free vaccination, the vaccine is often reimbursed by private insurance.
You can get the shingles vaccine directly at your local pharmacy. Your pharmacist or nurse can assess your vaccination needs and administer the vaccine, under certain conditions.
How is shingles treated?
For the best results, shingles treatment should be started as early as possible: ideally within three days of the first skin lesions appearing. You should see a doctor or your pharmacist as soon as you notice symptoms.
Shingles is treated with an antiviral, i.e., a drug that targets the virus. Under certain conditions, your pharmacist may prescribe this antiviral if your symptoms are clearly indicative of shingles. In addition, if you are experiencing pain, you can take painkillers to improve your quality of life during the acute phase of shingles.
You can also try a few non-medication strategies to help ease your symptoms and prevent complications from shingles:
- Apply cold compresses to the rash
- Gently clean the blisters and keep them dry
- Do not scratch or burst the blisters
- Wear loose, breathable clothing to reduce friction
- Get lots of rest
Other pain medications may be prescribed if pain persists after the acute phase of shingles (post-shingles neuralgia).
Shingles: An unpredictable but treatable disease
Shingles can develop without warning, but fortunately there are ways of treating it effectively. Recognizing the first symptoms early and getting vaccinated are the two best ways to reduce risks and complications.
Your Brunet-affiliated pharmacist is there to answer your questions, assess your situation, and advise you on the treatment best suited to your situation.
Last updated on March 24, 2026
Other articles that might interest you

